

Strengthening health systems, one family at a time
What would happen to health outcomes if caregivers had access to basic, life-saving skills?
I was raised by a strong grandmother who played a formative role in making me who I am today. She taught me how to read, do math, and sing Bangla classical music, among many other things. As I grew older, however, her strength began to fade as she suffered from a neurological condition. I was at the age where I did not understand much about her medical care, but as we went together to her many doctors’ appointments, I noticed my mother always carrying a set of heavy folders. She would keep it updated with copies of every doctor’s note, meticulously categorized and filed away. At home, she would create physical therapy diagrams, color-code and organize medications, and carefully prepare nutritious meals.
My grandmother had some great physicians managing her condition — but the person who actually enabled her to heal was my mother.
Years later in medical school, when it came time to discharge a patient, I noticed how uncomfortable I felt when we didn’t have the time to clearly explain the patient’s care to their loved ones. After all, as I knew all too well in the case of my own grandmother, it is up to the patient’s family to provide care when they return home.
My discomfort only grew when I visited healthcare settings in India and Bangladesh. Here nurses and doctors have even less time to spend with patients, and there is a greater distance and disconnect between hospitals and homes. At the same time, what was even more evident was the important — yet untapped — role of families in providing care. I began to wonder: Was there a way health systems could better leverage the love and care people provide for their families, especially in lower resource settings? In time, this question became a mission, and we started Noora Health in pursuit of a solution.
A gap in the healthcare system
The moment when a patient is discharged from hospital is often rushed. Despite their best intentions, staff have little time to convey proper care instructions, often leaving patients (and their loved ones) unclear on what to do next.

Though they are unprepared to take care into their own hands at home, caregivers frequently step up and fill this void left by overburdened health systems. But in the absence of the right information and skills, they sometimes miss critical warning signs. The result? A wound becoming infected or a newborn suffering from jaundice. Complications and hospital readmissions further burden families and healthcare systems and lead to tragic, yet preventable, illness and death. There are nearly 1.5 million under-5 deaths per year in South Asia alone, many of which can be averted through health practices that are actionable at home.
This gap in caregiver training is global, but is further exacerbated in low- and middle-income countries like India or Bangladesh where there are fewer healthcare workers and resources.
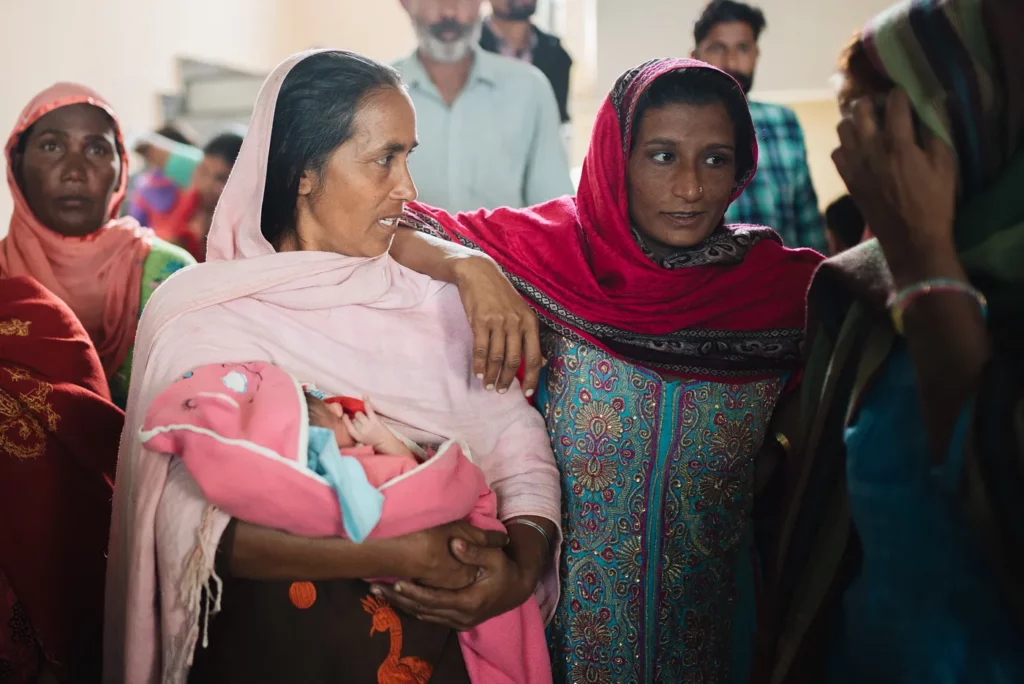
The power of families
What would happen if caregivers — these compassionate and capable resources — had access to basic, life-saving skills?
Research conducted on two unique patient populations in India — adult surgical patients and newborns and new mothers — suggests that sufficient training can equip family caregivers with the skills to improve health outcomes. Another study focused on ICU patients shows that the regular presence of family members not only meets the emotional needs of both families and patients, but also quickens recovery and helps reduce the duration of the ICU stay.
Not only does caregiver training improve health outcomes for the patient, it also helps reduce the mental load of caregiving carried by families. Globally, the burden of care falls disproportionately on women. It is estimated that 70 percent of caregivers are women and girls. The road to changing this is a long one, but what caregiver training does is that it provides an opportunity to share the load by involving other loved ones in the provision of care and make the process less scary, confusing, and stressful.
Similarly, caregiver training doesn’t mean that they are expected to replace doctors or nurses. But with the right knowledge, skills, and resources, caregivers can provide basic care, and reach out to the health system in moments of critical need. We saw the importance of adequately equipping and leaning on families to support care at home during the COVID-19 pandemic, where we faced a highly transmissible respiratory virus and overburdened health facilities.
Families are more than capable of handling a patient’s care, especially when they have resources and support tailored to their contexts and needs.
I’m reminded of a wife who received training on how to help her husband recover after a heart surgery. A few days later, we met her in the ward. She was beaming as we approached and shared how she had not been formally educated but the training was one of the first times someone had taken the time to teach her about health in a language that she understood. She proudly showed us a tracker of all of the caregiving tasks she had completed — physical therapy, tracking input/output, and vitals. When a new patient was admitted to the next bed, she also shared this information with their family members! In that moment, I realized that caregiving transcends any artificial limitations on acquiring knowledge or skills that we may place on people.
The foundations of family caregiver training
Effective caregiver training should be:
- Empathetic: Patients and their caregivers might be under intense pressure, and in the case of certain illnesses such as tuberculosis, often face stigma. Rather than making assumptions, it’s important to start by listening and understanding people’s experiences, and then meeting them where they are. For instance, when talking to families of pediatric cardiac surgery patients, we repeatedly heard them worrying about how the surgery would impact their child’s future potential in school and took steps to discuss this in our training.
- Comprehensive: When designing health education or behavior change programs for communities with low formal literacy, there is an assumption that it needs to be short and entertaining to keep people interested. There’s no doubt that the messaging needs to be well designed, but when it comes to caregiving, relying only on memes and short videos does a disservice to the capacity of individuals to comprehend the complexity of caregiving. And so, caregiver training needs to be comprehensive and talk about the why of a behavior, not just the how. Not only does this increase uptake, it also builds trust in the health system and the long-term capacity of caregivers.
- Timely: There are many critical questions that crop up once a patient has left the hospital. In moments like this information needs to be readily accessible to caregivers, allowing them to make informed decisions. Training programs must provide access to the information and live support efficiently — there are technologies over WhatsApp or automated response systems that can be used to provide this service, at scale.
- Actionable: Training should not just provide conceptual information on what diabetes is, for example, but also tell the caregiver what actionable steps they can take to support the patient. What family caregivers need most is the answer to one question: “What do I do now to keep my patient safe?”
- Contextual: Every community has their own unique resources and it’s important to tailor training to leverage said resources. The recommended diet for a patient in recovery, for instance, will not be followed if it doesn’t fit the family’s budget and locally available foods. Similarly, be clear, specific, and localize your advice on how to access care. In case of an urgent issue, in some places the first port of call will be the community health worker, and in others the nearest hospital.
- Safe: Caregiving can place significant stresses on the family caregiver, both physically and emotionally. Guide the caregiver on how to stay well and care for themselves as well.

Building the system
When I think back to my mother’s experience, even with the most advanced medical treatment, the onus was on her to figure out my grandmother’s care. And yet, her commitment is not an anomaly. Let’s use this moment to recognize that every family caregiver is an untapped resource, and they are ready to answer the call with skill and love.
A version of this article was originally published on July 13, 2020 and edited and updated in July 2023.



